Your blood pressure is silently doing one of two things right now — protecting your kidneys or destroying them. As a urologist, I see the consequences of uncontrolled hypertension every week: men in their 50s presenting with chronic kidney disease (CKD) that could have been prevented with a $40 monitor and five minutes a day. The tragedy is always the same — they didn’t know their blood pressure was high because they never measured it.
Buying a home blood pressure monitor is one of the highest-return health investments a man can make. But here’s the problem: most monitors on Amazon are not clinically validated, wrist monitors are unreliable, and even a good device produces inaccurate readings if you use it incorrectly. I’ve had patients bring me home readings of “110/70” while my clinic mercury sphygmomanometer shows 165/100. The device wasn’t broken — their technique was.
This review cuts through the marketing noise. I’ll tell you which monitors are actually validated against clinical-grade devices, which features genuinely matter (and which are gimmicks), and exactly how to measure your blood pressure so the number you get is one you can trust.
Download Your Free Clinical Action Plan
Enter your email below to download Dr. Khalid’s complete Blood Pressure & Kidney Protection Guide as a free, printable PDF.
📋 Key Takeaways
- Upper-arm cuffs are the only type recommended by ESH, AHA, and NICE — wrist and finger monitors are not clinically reliable enough for home use.
- A monitor must carry AMA VDL, ESH, or AAMI validation — without this, the readings are meaningless regardless of brand prestige.
- The Omron Silver is my top pick for most men — validated, affordable, and includes advanced averaging features.
- Proper technique matters more than the device — sitting upright, feet flat, arm supported at heart level, empty bladder, no talking, and five minutes of rest.
- Home readings above 135/85 mmHg are considered hypertensive — this threshold is lower than the clinic threshold of 140/90 because home readings naturally run lower.
- Uncontrolled hypertension is the second leading cause of kidney failure worldwide — home monitoring is the single most effective way to catch it early.
In This Guide:
Why Every Man Over 35 Needs a Home Blood Pressure Monitor
Hypertension affects approximately 1.3 billion adults worldwide, and nearly half of them don’t know they have it [1]. The condition earns its reputation as the “silent killer” honestly — there are no reliable symptoms until organ damage has already occurred. By the time a man notices headaches, visual changes, or ankle swelling, his kidneys, heart, or brain may have sustained years of cumulative injury.
In my urology practice, I see the downstream consequences. Hypertensive nephrosclerosis — kidney damage caused purely by chronically elevated blood pressure — is the second leading cause of end-stage renal disease (ESRD) in Europe and North America, behind diabetes [2]. These men often had no idea their blood pressure was elevated because they relied on occasional GP readings, which introduce two major sources of error: white-coat hypertension (artificially high readings from clinic anxiety) and masked hypertension (normal clinic readings that hide persistently high pressures at home).
Home blood pressure monitoring (HBPM) eliminates both problems. The European Society of Hypertension (ESH) 2023 guidelines now recommend HBPM as an integral part of hypertension management — not an optional extra [3]. Multiple large studies have shown that home readings are actually better predictors of cardiovascular events and kidney damage than clinic readings [4].
➡️ Related Read: High Blood Pressure and Your Kidneys: The Silent Damage Nobody Talks About
What Makes a Blood Pressure Monitor “Clinically Validated”?
This is the single most important concept in this article, and the one most people ignore. A clinically validated monitor has been independently tested against a mercury sphygmomanometer (the gold standard) using a standardised protocol. In the US, the gold standard list is the US Blood Pressure Validated Device Listing (VDL). Devices are tested using the Association for the Advancement of Medical Instrumentation (AAMI) standard or the ESH International Protocol [5]. These protocols require the device to produce readings within ±5 mmHg of the reference standard.
A monitor that is NOT validated may look identical to one that is. It has a cuff, a screen, a button. It gives you a number. But that number could be 10–20 mmHg off — enough to classify a hypertensive patient as normal, or a normotensive patient as hypertensive. I’ve seen both scenarios in my clinic, and both are dangerous: one leads to missed treatment, the other to unnecessary medication with side effects.
Before buying any monitor, verify it exists on the US VDL database (validatebp.org). If the device isn’t on it, don’t buy it — regardless of how many Amazon reviews it has.
Why Wrist Monitors Are Not Recommended
Wrist monitors are convenient, but their accuracy is highly position-dependent. The wrist must be held at exact heart level during measurement — even a few centimetres too high or too low introduces significant error [6]. Most people hold wrist monitors in their lap or let their arm hang, which inflates the reading. The ESH, AHA, and NICE all recommend upper-arm cuff monitors as the standard for home use. Wrist monitors are acceptable only when the upper arm is too large for available cuffs — and even then, they must be validated models used with strict positioning technique.
Features That Actually Matter (and What’s Marketing)
Blood pressure monitor manufacturers love to add features. Some of these are clinically useful. Most are not. Here’s how to separate signal from noise.
Features Worth Paying For
Clinically validated accuracy — non-negotiable. This is the baseline. If a device lacks VDL/ESH validation, no other feature compensates for unreliable readings.
Irregular heartbeat detection (IHB) & AFib detection — genuinely useful. Atrial fibrillation (AF) affects roughly 2% of adults under 65 and 9% over 65 [7]. A monitor with an AF or IHB detection algorithm can flag irregular rhythms during routine measurements. This is not a diagnostic tool — it won’t replace an ECG — but it has identified asymptomatic AF in screening studies, prompting referral and anticoagulation that prevented strokes.
Appropriate cuff size range — critical for accuracy. A cuff that is too small over-reads; a cuff that is too large under-reads. Most standard cuffs fit arm circumferences of 9 to 13 inches. If your upper arm measures over 13 inches (common in muscular or overweight men), you need a wide-range or large/XL cuff (up to 17 inches) — either included or available as an accessory.
Memory storage for 60+ readings — allows you to track trends over weeks and share meaningful data with your doctor, rather than presenting a single snapshot reading.
Features That Are Nice but Not Essential
Bluetooth/app connectivity — convenient for long-term graphing and sharing data with your doctor digitally, but not necessary if you’re willing to use a paper log.
Multi-user profiles — useful if two people share the same device. Not relevant for a single user.
Averaging function — some monitors automatically average the last three readings. This is helpful because guidelines recommend averaging multiple readings. But you can do this manually with a calculator.
Features That Don’t Matter
Colour-coded displays — these traffic-light systems (green/amber/red) are based on arbitrary thresholds that may not match your doctor’s target. They can create unnecessary anxiety or false reassurance.
Voice readout — a gimmick. If you can see a screen, you don’t need a robot reading your numbers aloud.
“Medical grade” marketing language — this phrase has no regulated meaning. Only VDL/validation status matters.

My Top 3 Blood Pressure Monitors for Home Use (US Market)
I’ve selected these three monitors based on four criteria: clinical validation status (US VDL listed), accuracy in independent testing, practical usability, and value for money.
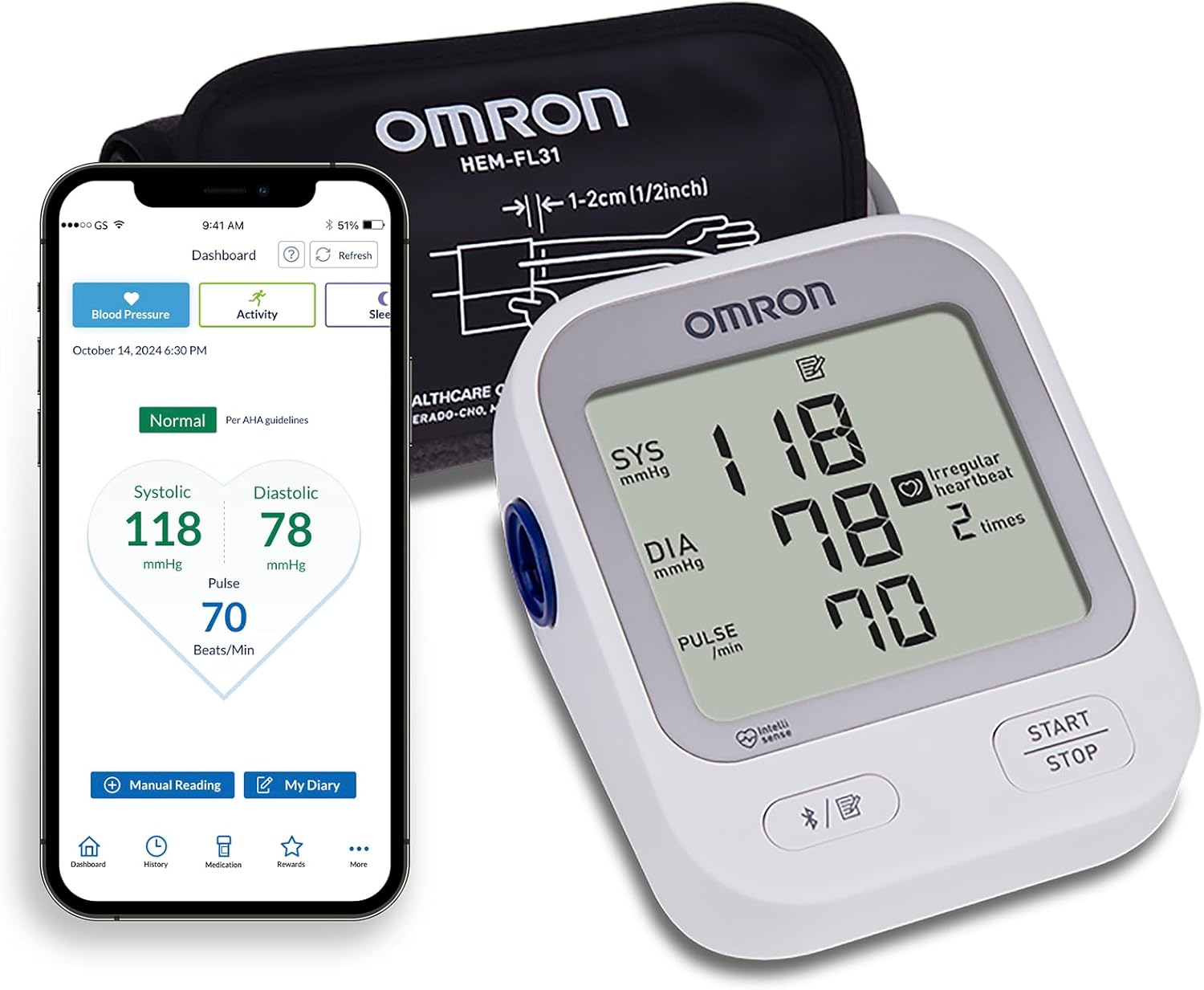
Omron Silver (BP5250)
US VDL Validated · Advanced Averaging
The Omron Silver is an excellent baseline choice. It is fully validated on the US Blood Pressure Validated Device Listing (VDL) and features an advanced averaging capability. The included wide-range D-ring cuff fits arms 9 to 17 inches, covering most men without needing a separate extra-large cuff.

Omron Platinum (BP5450)
US VDL Validated · AFib Detection Indicator
If you want digital tracking and the ability to share readings with your doctor via an app, the Platinum model is the natural upgrade. Crucially, it includes an evidence-based atrial fibrillation (AFib) screening algorithm alongside dual-display technology that compares your current reading to your previous one.

A&D Medical Premium (UA-767F)
US VDL Validated · Irregular Heartbeat Detection
A&D Medical is highly respected in clinical settings. This model is rigorously validated on the US VDL and includes an Irregular Heartbeat (IHB) detection feature. It is a fantastic, robust alternative to Omron if you want medical-grade accuracy without paying extra for Bluetooth or app connectivity.
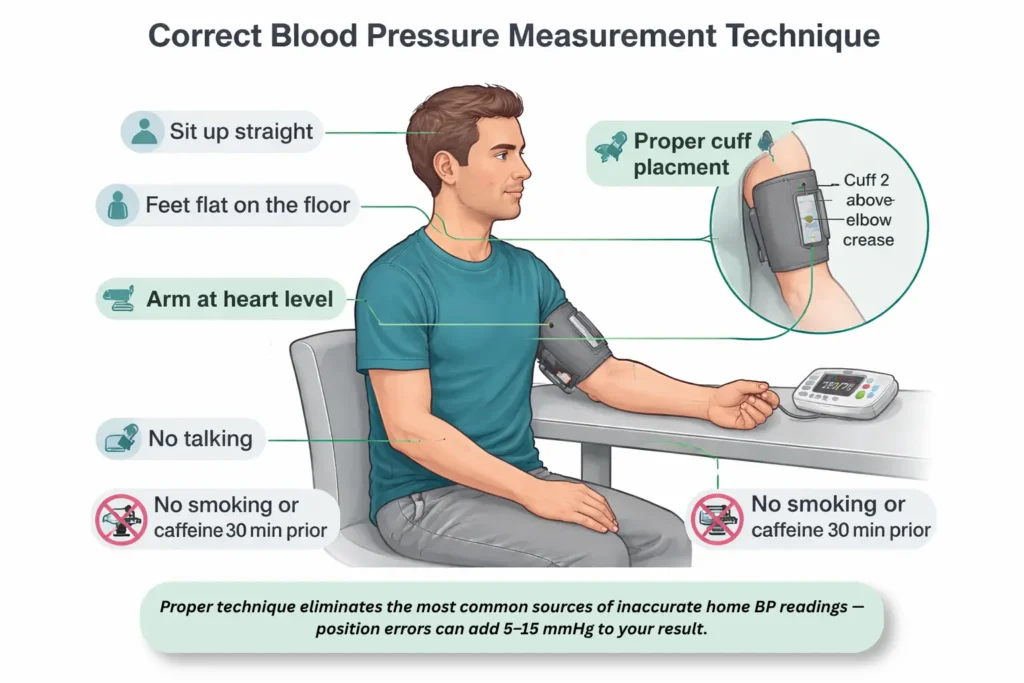
How to Measure Blood Pressure Correctly at Home
An excellent monitor with poor technique gives you garbage data. I’ve seen patients with perfectly normal blood pressure convinced they’re hypertensive because they measured after climbing stairs, with a full bladder, while sitting on a sofa with their legs crossed. Every one of those errors inflates the reading by 5–15 mmHg — and they’re cumulative [11].
Follow this protocol every time:
Step-by-Step Measurement Protocol
1. Timing: Measure at the same time each day — ideally morning (before medication) and evening. Avoid measuring within 30 minutes of exercise, caffeine, smoking, or a large meal.
2. Position: Sit in a chair with a back support. Feet flat on the floor — never crossed. Arm supported on a table or armrest at heart level. The cuff should be on bare skin, not over clothing.
3. Rest first: Sit quietly for 5 full minutes before pressing the button. No talking, no phone, no television. This rest period is the most commonly skipped step — and skipping it can add 5–10 mmHg to systolic readings.
4. Cuff placement: Bottom edge of the cuff should sit about 1 inch above the elbow crease. The artery marker on the cuff (usually a line or arrow) should align with the brachial artery on the inner arm.
5. Take two readings: Measure twice, one minute apart. Record the average of the two readings. If the first two differ by more than 10 mmHg systolic, take a third and average the last two.
6. Record everything: Write down the date, time, systolic, diastolic, and pulse in a log. If your doctor asks for home readings, provide at least 12–14 paired readings (morning and evening over 7 consecutive days), discarding the first day’s measurements [12].
Understanding Your Home Readings: What the Numbers Mean
Home blood pressure thresholds are different from clinic thresholds. Because home readings are generally lower than clinic readings (no white-coat effect), the cut-off for hypertension at home is 135/85 mmHg, not the 140/90 mmHg used in clinics [3]. This is a crucial distinction that many patients — and some doctors — miss.
Optimal home BP: Below 120/80 mmHg — excellent.
Normal home BP: 120–134/80–84 mmHg — acceptable for most people, but warrants monitoring if you have kidney disease or diabetes (where targets are stricter).
Home hypertension: 135/85 mmHg or above — this warrants a conversation with your doctor about lifestyle modification and possibly medication.
Urgent: Any reading above 180/120 mmHg at home — if accompanied by headache, chest pain, visual changes, or breathlessness, this constitutes a hypertensive emergency. Attend the emergency room immediately. If asymptomatic, repeat the measurement after 5 minutes of rest. If still above 180/120, contact your physician urgently the same day.
The BP-Kidney Connection: Why Urologists Care About Your Blood Pressure
You might wonder why a urologist is writing about blood pressure monitors. The answer is straightforward: the kidneys are the organ most damaged by uncontrolled hypertension after the brain and heart. The glomeruli — the microscopic filtering units inside each kidney — are exquisitely sensitive to pressure. Chronically elevated blood pressure thickens and narrows the afferent arterioles (the tiny blood vessels feeding each glomerulus), gradually reducing filtration capacity. This process, called hypertensive nephrosclerosis, is irreversible once established [2].
I see this regularly. A man comes in for kidney stone follow-up or haematuria (blood in urine) investigation. His blood work reveals a raised creatinine and reduced eGFR (estimated glomerular filtration rate) — markers of kidney function decline. When I ask about his blood pressure, he says “it’s been a bit high but I don’t take tablets.” He’s 54 and already has Stage 3 CKD. Had he been monitoring at home and treated five years earlier, much of that damage would have been preventable.
➡️ Related Read: High Blood Pressure and Your Kidneys: The Silent Damage Nobody Talks About
Common Blood Pressure Myths That Mislead Men
Myth: “I Feel Fine, So My Blood Pressure Must Be Normal”
This is the most dangerous misconception. Hypertension at levels of 150–170 systolic rarely produces symptoms. By the time symptoms appear — headaches, nosebleeds, visual disturbance — the blood pressure is typically severely elevated (above 180–200 systolic) and organ damage is already in progress. You cannot feel blood pressure. You can only measure it.
Myth: “One High Reading Means I Have Hypertension”
A single elevated reading is not a diagnosis. Blood pressure fluctuates throughout the day by 20–30 mmHg depending on activity, stress, hydration, and time of day [13]. That’s precisely why home monitoring over 7 days (with averaged readings) is more reliable than a single clinic snapshot. Don’t panic over one reading — track the trend.
Myth: “My Wrist Monitor Is Just as Good”
It isn’t. Even validated wrist monitors introduce position-dependent errors that upper-arm cuffs largely avoid. Unless you have a physical reason preventing upper-arm measurement, always use an upper-arm oscillometric cuff for home monitoring.
➡️ Related Read: How to Lower Blood Pressure Naturally: What Actually Works
How Often Should You Monitor at Home?
This depends on your clinical situation:
Newly diagnosed or starting/changing medication: Measure twice daily (morning and evening) for 7 consecutive days. Discard the first day’s readings (they’re typically elevated from anxiety) and average the remaining 12 readings. Share this with your doctor at your next review [12].
Stable on medication: Measure for one week per month. This gives your doctor an ongoing trend without creating measurement fatigue.
Healthy with no diagnosis: Check quarterly or whenever you have a routine appointment. If you have risk factors (family history, obesity, diabetes, kidney disease, high salt diet), increase to monthly spot checks.
Cuff Size: The Accuracy Factor Most People Ignore
Using the wrong cuff size is one of the most common — and most consequential — sources of home monitoring error. A cuff bladder that is too small will overestimate blood pressure by up to 10–30 mmHg [14]. A cuff that is too large will underestimate. This means a muscular man using a standard 9-13 inch cuff when his arm measures 15 inches may be falsely classified as hypertensive and started on medication he doesn’t need.
How to measure your arm: Wrap a tape measure around the midpoint of your upper arm (halfway between shoulder and elbow). If the circumference is below 9 inches, you need a small cuff. If between 9 and 13 inches, a standard cuff. If above 13 inches, a wide-range or large cuff (13–17 inches). Many premium monitors in the US now include wide-range cuffs that cover 9 to 17 inches — the Omron D-ring cuff is one example.
➡️ Related Read: Renal Hypertension: When Your Kidneys Are Secretly Raising Your BP
💡 In My Practice
In my practice, the most common scenario I encounter is a man told his blood pressure is “borderline” by his primary care physician, but who has never measured it at home. When I ask him to track it for a week using a validated upper-arm device like the Omron Silver, the data provides absolute clarity. Either it confirms the elevation and he accepts treatment readily because he has seen the evidence himself, or it reveals white-coat hypertension, sparing him from unnecessary medication.
More concerning are the men relying on cheap, unvalidated wrist monitors. Recently, I saw a 54-year-old man with microalbuminuria and a declining eGFR. He confidently reported his home BP was “always 120/75.” When we measured it in the clinic using a calibrated device, it was 162/98. The false reassurance from his inaccurate wrist monitor cost him years of early, nephroprotective treatment. This is exactly why I insist my patients invest in an AMA VDL-validated upper-arm monitor. The $50 spent on a reliable device is insignificant compared to the cost of dialysis.
⚠️ When to See a Doctor — Urgently
- Home readings consistently above 180/120 mmHg — this constitutes a hypertensive crisis. If accompanied by symptoms (headache, chest pain, visual changes, breathlessness, nosebleed), attend the emergency room immediately.
- Home readings consistently above 150/95 mmHg despite medication — this indicates resistant or poorly controlled hypertension and may require specialist referral, medication adjustment, or investigation for secondary causes.
- New ankle swelling, foamy urine, or reduced urine output — these may signal kidney damage from chronically elevated blood pressure and warrant urgent blood and urine tests.
- Sudden large drop in BP with dizziness or fainting — may indicate overmedication, dehydration, or cardiac arrhythmia. Seek same-day medical review.
- Monitor consistently flagging irregular heartbeat — while not a diagnosis, repeated IHB or AFib alerts warrant an ECG to rule out atrial fibrillation, especially in men over 65.
Frequently Asked Questions
How accurate are home blood pressure monitors compared to the ones at the doctor’s office?
A clinically validated home monitor (US VDL, ESH, or AAMI certified) is accurate to within ±5 mmHg of a mercury sphygmomanometer — the same gold standard your doctor’s manual device is calibrated against. The key phrase is “clinically validated.” Unvalidated monitors sold online can be off by 10–20 mmHg. Home readings are actually more representative of your true blood pressure than clinic readings because they’re taken in your natural environment, without the anxiety of a medical setting. Multiple studies, including the Ohasama and Finn-Home studies, have shown that home readings are better predictors of cardiovascular events and organ damage than clinic readings [4].
Should I buy a wrist blood pressure monitor or an upper-arm one?
Upper-arm, always. Every major guideline body — AHA, ESH, NICE, and BHS — recommends upper-arm cuff monitors for home use. Wrist monitors are highly sensitive to arm position: if your wrist is even a few centimetres above or below heart level, the reading shifts significantly. Most people hold wrist monitors in their lap (too low, overestimates BP) or on a table (often too high, underestimates BP). The only legitimate reason to use a wrist monitor is if your upper arm circumference exceeds the range of available cuffs — and even then, you need a validated wrist model used with strict positioning.
Why is my home blood pressure reading different from the one at my physician’s clinic?
This is expected and well-documented. White-coat hypertension — where clinic readings are elevated but home readings are normal — affects up to 30–40% of people diagnosed with hypertension in a clinic setting [15]. The reverse phenomenon, masked hypertension (normal clinic, elevated at home), affects approximately 10–15%. This is precisely why home monitoring is so valuable: it captures your “real” blood pressure in your natural environment. The diagnostic threshold differs too — hypertension at home is ≥135/85 mmHg, while in the clinic it’s ≥140/90 mmHg, because home readings naturally run slightly lower.
Can a blood pressure monitor detect atrial fibrillation?
Some validated monitors, such as the Omron Platinum, include irregular heartbeat detection (IHB) or specific AFib indicator algorithms. These are screening tools, not diagnostic devices — a positive alert means you should get an ECG from your doctor to confirm. But given that AFib often causes no symptoms and is a leading cause of stroke, catching it incidentally during a blood pressure check is genuinely valuable, especially for men over 65.
How often should I replace my blood pressure monitor?
Most home blood pressure monitors remain accurate for 3–5 years with regular use, though this varies by manufacturer. Companies like Omron generally recommend recalibration or replacement every 2 years for clinical use, though home devices used less frequently may last longer. The cuff degrades faster than the monitor itself — bladder leaks, worn Velcro, and stretched fabric all reduce accuracy. If readings start seeming inconsistent or if the device is dropped, bring it to your next appointment and ask to have it checked against their calibrated device.
📚 References
- NCD Risk Factor Collaboration. Worldwide trends in hypertension prevalence and progress in treatment and control from 1990 to 2019. Lancet. 2021;398(10304):957-980.
- Udani S, Lazich I, Bhatt DL. Epidemiology of hypertensive kidney disease. Nat Rev Nephrol. 2011;7(1):11-21.
- Mancia G, Kreutz R, Brunström M, et al. 2023 ESH Guidelines for the management of arterial hypertension. J Hypertens. 2023;41(12):1874-2071.
- Niiranen TJ, Hänninen MR, Johansson J, et al. Home-measured blood pressure is a stronger predictor of cardiovascular risk than office blood pressure: the Finn-Home study. Hypertension. 2010;55(6):1346-1351.
- Stergiou GS, Palatini P, Parati G, et al. 2021 European Society of Hypertension practice guidelines for office and out-of-office blood pressure measurement. J Hypertens. 2021;39(7):1293-1302.
- Stergiou GS, Giovas PP, Neofytou MS, et al. Validation of the Microlife WatchBP Home wrist device for home blood pressure measurement. Blood Press Monit. 2007;12(3):185-188.
- Hindricks G, Potpara T, Dagres N, et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation. Eur Heart J. 2021;42(5):373-498.
- Topouchian J, Agnoletti D, Blacher J, et al. Validation of four automatic devices for self-measurement of blood pressure according to the international protocol of the European Society of Hypertension. Vasc Health Risk Manag. 2011;7:709-717.
- Akpolat T, Erdem E, Aydogdu T. Validation of the Omron M3 Intellisense (HEM-7051-E) upper arm blood pressure monitor, for self-measurement, according to the European Society of Hypertension International Protocol revision 2010. Blood Press Monit. 2012;17(2):97-101.
- Wiesel J, Fitzig L, Herschman Y, Messineo FC. Detection of atrial fibrillation using a modified Microlife blood pressure monitor. Am J Hypertens. 2004;17(8):727-731.
- Pickering TG, Hall JE, Appel LJ, et al. Recommendations for blood pressure measurement in humans: an AHA scientific statement. Hypertension. 2005;45(1):142-161.
- Parati G, Stergiou GS, Dolan E, Bilo G. Blood pressure variability: clinical relevance and application. J Clin Hypertens. 2018;20(7):1133-1137.
- Mancia G, Fagard R, Narkiewicz K, et al. 2013 ESH/ESC Guidelines for the management of arterial hypertension. J Hypertens. 2013;31(7):1281-1357.
- Palatini P, Benetti E, Fania C, et al. Effect of cuff size on clinical blood pressure measurement. J Hypertens. 2020;38(12):2359-2364.
- Banegas JR, Ruilope LM, de la Sierra A, et al. Clinic versus ambulatory blood pressure measurements in treated hypertensive patients. Hypertension. 2018;72(4):897-903.

Dr. Muhammad Khalid
MBBS · FCPS (Urology) · MCPS (Gen. Surgery) · CHPE · CRSM · IMC #539472
Specialist urologist with 11+ years of clinical experience across tertiary teaching hospitals. Trained at Lady Reading Hospital and Khyber Teaching Hospital, Peshawar. Author of 5 peer-reviewed international publications in Cureus, WJSA, and AJBS. Procedural expertise: URS, PCNL, RIRS, TURP, TURBT, and major open urological surgery. Full profile →
This article is for educational purposes only and does not constitute medical advice. Always consult your physician or urologist for diagnosis and treatment decisions specific to your condition.
