
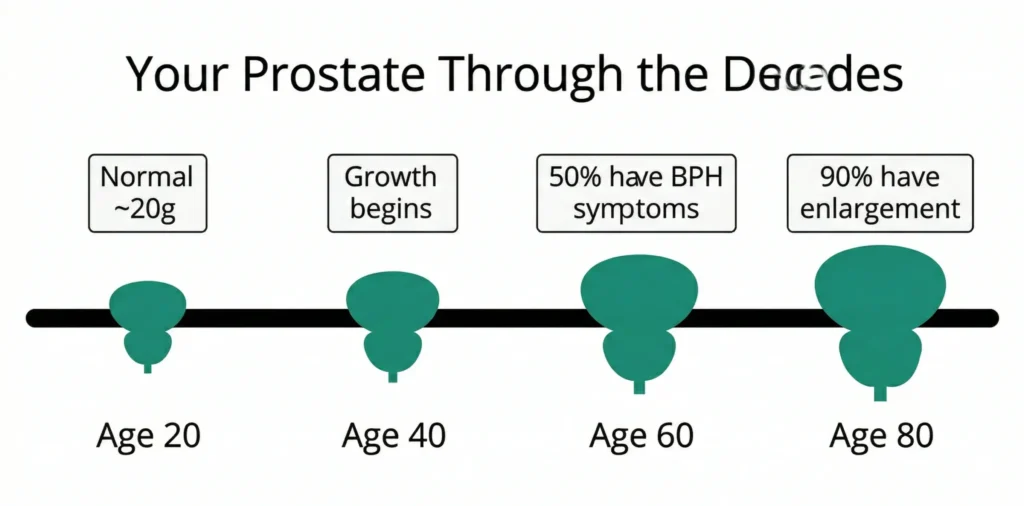
Here is the statistic most men over 40 have never been told: by age 60, half of all men have a prostate large enough to cause urinary symptoms. By age 85, that figure rises to 90% [1]. Yet the average man waits four to five years after noticing symptoms before seeing a doctor — years during which treatable problems quietly progress into complicated ones.
The prostate is not something to think about only when it becomes a problem. It is a gland that changes predictably with age, produces symptoms that are easy to misattribute to “just getting older,” and carries a screening test — the PSA — that generates as much confusion as it does reassurance. Understanding your prostate at 40 or 50 puts you firmly in control of what happens at 60 and 70.
This article is the guide I wish every man over 40 had before walking into my clinic. It covers anatomy, benign enlargement (BPH), prostate cancer screening, lifestyle, and when to act — without the jargon, without the unnecessary alarm, and without the watered-down vagueness that drives men straight back to Google for a second opinion.
Want to read this later?
Enter your email below to download Dr. Khalid’s complete Prostate Health Guide as a free, printable PDF.
📋 Key Takeaways
- Benign prostatic hyperplasia (BPH) — non-cancerous prostate enlargement — affects 50% of men by age 60 and is the most common cause of urinary symptoms in men over 40 [1]
- BPH and prostate cancer are entirely separate conditions. Having an enlarged prostate does not increase your cancer risk
- The PSA blood test is the cornerstone of early prostate cancer detection — men with a family history of prostate cancer should discuss baseline testing from age 40–45
- Most prostate cancer is slow-growing — not every cancer needs immediate treatment. Low-grade disease is increasingly managed with active surveillance rather than surgery
- Nocturia (getting up 2+ times per night to urinate) is the symptom that most commonly drives men to seek help — and it is also the most treatable
- Lifestyle changes — weight loss, caffeine and alcohol reduction, pelvic floor exercises — can meaningfully reduce urinary symptoms before any medication is needed
- Fever with urinary symptoms is a red flag requiring same-day assessment — it may indicate acute prostatitis or an infected obstructed kidney
What the Prostate Actually Does (Most Men Have No Idea)
The prostate is a walnut-sized gland — roughly 20–25 grams in young adulthood — that sits immediately below the bladder and wraps around the urethra like a ring around a pipe. Its primary function is reproductive: it produces the fluid component of semen that nourishes and transports sperm. During ejaculation, the prostate contracts and secretes this fluid into the urethra, where it mixes with sperm from the testes.
Its anatomical position is what makes it so clinically significant. The urethra runs directly through the prostate. When the prostate enlarges — as it does in virtually all men with age — it compresses this urethral channel from the outside, increasing resistance to urine flow. The bladder, which lies directly above, must work harder to push urine through the narrowing. Over years, this creates the classic constellation of lower urinary tract symptoms (LUTS) that most men over 60 recognise.
The three zones — why location matters
The prostate has three distinct anatomical zones, and understanding them clarifies why different diseases develop in the same gland:
Transition zone — the innermost zone surrounding the urethra. This is where benign prostatic hyperplasia (BPH) originates. The transition zone grows throughout adult life under the influence of dihydrotestosterone (DHT). It does not cause cancer.
Peripheral zone — the outer zone that makes up roughly 70% of the prostate’s volume. This is where approximately 70–80% of prostate cancers arise. It is also the zone assessed by digital rectal examination (DRE) — because it faces posteriorly towards the rectum [2].
Central zone — surrounds the ejaculatory ducts. A smaller proportion of tumours arise here; they tend to be more aggressive when they do.
The practical implication: BPH (transition zone) and prostate cancer (predominantly peripheral zone) are entirely separate diseases originating in different parts of the same organ. Having an enlarged prostate does not predispose you to cancer, and prostate cancer can develop in men with no symptoms of BPH whatsoever.
Benign Prostatic Hyperplasia (BPH): The Condition Nobody Warns You About
Benign prostatic hyperplasia — non-cancerous overgrowth of prostate tissue — is the most prevalent condition in ageing men. By age 60, 50% of men have histological BPH (microscopic enlargement). By age 85, that figure reaches 90% [1]. Yet a significant proportion of these men attribute their symptoms to “just getting older” and seek no treatment, when effective options exist at every stage of the disease.
What BPH actually feels like
BPH produces two categories of symptoms, both of which are scored clinically using the International Prostate Symptom Score (IPSS) — a seven-question tool where 0–7 is mild, 8–19 is moderate, and 20–35 is severe. This is the first thing I assess in every BPH patient.
Find Out Your Exact IPSS Score
Don’t guess how severe your urinary symptoms are. Use our interactive, clinically validated IPSS Calculator to get your precise score in under 60 seconds.
Storage symptoms (often the most bothersome):
Nocturia — waking two or more times per night to urinate. This single symptom drives the majority of men to their GP, because it directly destroys sleep quality. Urgency — a sudden, strong urge to urinate that is difficult to defer. Frequency — needing to urinate more than eight times in 24 hours. Urge incontinence — leaking before reaching the toilet.
Voiding symptoms (the classic obstructive signs):
Weak or reduced stream. Hesitancy — waiting and straining before the stream starts. Intermittency — the stream stopping and starting. Terminal dribbling — a slow trickle at the end of voiding. The sensation of incomplete emptying, which may be confirmed by post-void residual measurement on ultrasound.
The pattern matters clinically. A man with predominantly storage symptoms may have an overactive bladder rather than — or in addition to — BPH. A man with predominantly voiding symptoms almost certainly has a bladder outlet obstruction. Getting this distinction right determines the treatment approach.
Why BPH is not just an inconvenience
Left untreated, progressive BPH can cause consequences far beyond inconvenient bathroom trips. Acute urinary retention — the sudden, complete inability to urinate — occurs in roughly 2% of men per year once BPH is established, and requires emergency catheterisation [3]. Recurrent urinary tract infections develop when the bladder fails to empty completely and stagnant urine becomes infected. Bilateral hydronephrosis — back-pressure from persistent obstruction — can silently damage both kidneys over years. And bladder detrusor failure, where the overworked bladder muscle eventually loses its contractile strength, may not be reversible even after successful surgery.
These are not rare outcomes. They are the natural history of untreated moderate-to-severe BPH in a significant proportion of men who delay seeking assessment.
➡️ Related: Enlarged Prostate (BPH) — When Medication Fails and Surgery Becomes the Answer
Prostate Cancer Screening: What Every Man Over 40 Needs to Know
Prostate cancer is the most common non-skin cancer in men — approximately 1 in 8 men will receive a diagnosis during their lifetime [4]. It is also one of the most survivable cancers when detected early. The five-year survival rate for localised prostate cancer exceeds 99% [4]. The men who die from prostate cancer are predominantly those diagnosed late, with high-grade or metastatic disease that was not caught during a window of curability.
This is not an argument for blanket screening of every man regardless of risk. It is an argument for informed, risk-stratified screening — knowing your personal risk and acting accordingly.
The PSA test: what it is and what it is not
PSA (prostate-specific antigen) is a protein produced by the prostate gland. A simple blood test measures its concentration in the bloodstream. When the prostate is enlarged, inflamed, or cancerous, more PSA leaks into the blood and the measured level rises.
The most important thing to understand about PSA: it is prostate-specific, not cancer-specific. PSA can be elevated by BPH, prostatitis, a urinary tract infection, recent vigorous exercise, cycling, and ejaculation within 48 hours of the test. A raised PSA is not a cancer diagnosis — it is a signal that warrants further investigation [5].
Confused by your PSA lab results?
Because normal PSA levels change as you age, a raw number can be misleading. Enter your age and PSA level into our interpreter to see if you fall into the normal, grey zone, or high-risk category.
The traditional “normal” cutoff of 4.0 ng/mL is a blunt instrument. Modern PSA interpretation uses four parameters, not one number in isolation: the absolute PSA value adjusted for age, the rate of change over time (PSA velocity — a rise of more than 0.75 ng/mL per year is concerning regardless of absolute level), the free-to-total PSA ratio (cancer produces more bound PSA, so a low free fraction raises suspicion), and PSA density (PSA divided by prostate volume — a large benign prostate will naturally produce more PSA than a small one).
When to start — the age-by-age framework
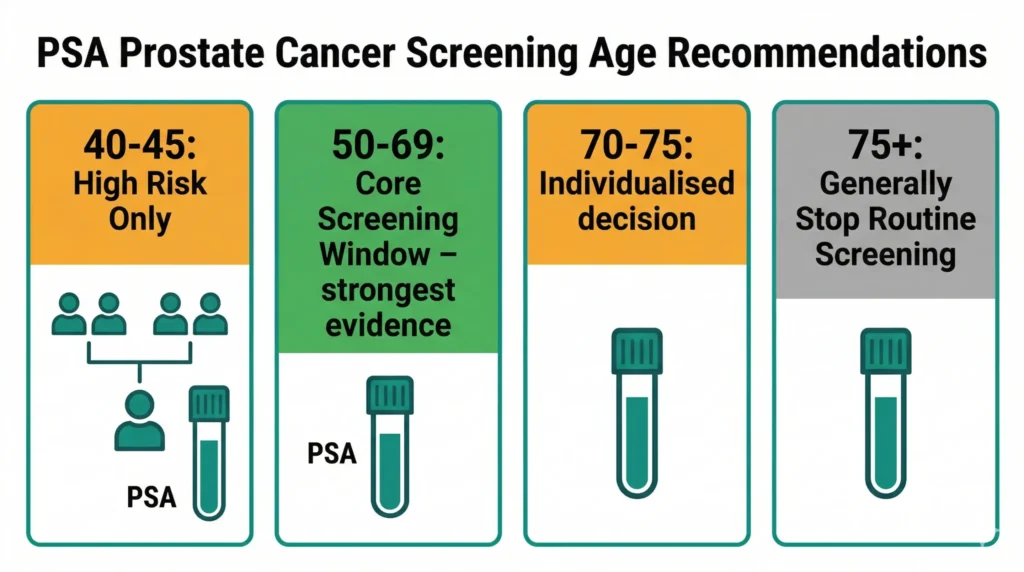
Screening recommendations differ by risk group, and one-size-fits-all advice is genuinely unhelpful here:
Ages 40–45 (high-risk men only): Men with a first-degree relative (father or brother) diagnosed with prostate cancer, men of African or Caribbean descent, and known BRCA2 mutation carriers should discuss a baseline PSA test at this age. A PSA below 1.0 ng/mL at 40–45 predicts a very low lifetime risk of clinically significant cancer — repeat testing can be deferred for years. A PSA above 1.0 ng/mL warrants closer monitoring [6].
Ages 50–69 (average-risk men): This is where the strongest evidence for screening benefit lies. The ERSPC trial — the largest prostate cancer screening study ever conducted — demonstrated a 20% reduction in prostate cancer mortality in men screened in this age band [7]. PSA testing every two years is the recommended frequency for men with PSA below 2.0 ng/mL. Annual testing is preferred if PSA is 2.0–3.0 ng/mL.
Ages 70–75 (individualised): Screening benefit must be weighed against life expectancy and competing health risks. Men in excellent health with a 10+ year life expectancy may benefit from continued monitoring, particularly if previous PSA values were elevated or rising.
Ages 75+: Routine PSA screening is generally not recommended. Prostate cancer is typically slow-growing, and the lead time between diagnosis and cancer-specific death for localised disease often exceeds the remaining life expectancy in this age group [6].
➡️ Related: Prostate Cancer Screening — The Age-by-Age Guide Every Man Needs
Understanding the PSA Grey Zone: When Results Cause More Anxiety Than Answers
The most common scenario that drives men into my consulting room in an anxious state: a GP phone call to say “your PSA is slightly raised — I’m referring you to urology.” The man goes home, searches online, and arrives at his urology appointment having already read about biopsies, Gleason scores, and survival statistics.
Here is what most of those men are never told at the point of referral: in the PSA grey zone of 4–10 ng/mL, 75% of biopsies find no cancer whatsoever. Three out of four men with an elevated PSA in this range have a benign explanation — most commonly BPH, prostatitis, or an uncorrected confounding factor before the blood draw [5].
And if cancer is found — the majority of grey-zone cancers are low-grade (Gleason 6 / Grade Group 1), slow-growing tumours that can be safely monitored rather than immediately treated. The pathway from “elevated PSA” to “urgent surgery” is far less common than online reading suggests, and modern investigation tools — particularly multiparametric MRI — have made that pathway far more selective and accurate than it was even five years ago.
➡️ Related: My PSA is 4.5 — Do I Have Cancer? Understanding ‘Grey Zone’ Results
Prostatitis: The Third Prostate Condition (And the Most Often Missed)
Prostatitis — inflammation or infection of the prostate — is the third major prostate condition and the one most commonly misunderstood. It is not just a condition of older men. Prostatitis accounts for roughly 8% of all outpatient urology visits, and chronic prostatitis / chronic pelvic pain syndrome (CP/CPPS) is particularly prevalent in men aged 25–45 [8].
The four categories
Acute bacterial prostatitis is a urological emergency — fever, rigors, severe perineal pain, and lower urinary symptoms in a systemically unwell man. It requires IV antibiotics and hospital admission in severe cases. PSA can spike dramatically during an episode, sometimes to 20–30 ng/mL or higher. A PSA test drawn during or within six weeks of acute prostatitis is entirely uninterpretable for cancer screening purposes.
Chronic bacterial prostatitis presents with recurrent UTIs in men, caused by bacteria persisting in the prostate gland. It requires prolonged antibiotic therapy (typically 4–6 weeks of a fluoroquinolone) because prostatic tissue is poorly penetrated by many antibiotics.
Chronic prostatitis / chronic pelvic pain syndrome (CP/CPPS) — the most common category — produces perineal, scrotal, or lower abdominal pain or discomfort for at least three of the past six months, in the absence of proven infection [8]. It frequently coexists with voiding symptoms and sexual dysfunction, and can cause young men to genuinely believe they have cancer. The diagnosis is clinical; treatment is multimodal and often frustrating.
Asymptomatic inflammatory prostatitis — found incidentally on biopsy or semen analysis with no symptoms. No treatment is required.
Diet, Lifestyle, and Prostate Health: What the Evidence Actually Shows
This is where patient expectations most frequently diverge from the clinical evidence. Men arrive having read about “superfoods” for prostate health, miracle supplements, and dietary protocols that claim to shrink an enlarged prostate or prevent cancer. The honest answer is more nuanced — some lifestyle factors have genuine supporting evidence, many do not.
What has good evidence
Weight management: Obesity is associated with larger prostate volume, more severe LUTS, and higher-grade prostate cancer at diagnosis [9]. This is one of the most consistent findings in the prostate health literature. Reducing BMI to below 27 is associated with measurable improvements in urinary symptom scores in men with BPH.
Physical activity: A systematic review of 11 prospective studies found that physically active men have significantly lower rates of BPH symptom progression and lower prostate cancer incidence compared to sedentary men [10]. The mechanism appears to involve reduced sympathetic tone (which relaxes the smooth muscle in the prostate and bladder neck) and improved insulin sensitivity. Thirty minutes of brisk walking five times weekly is sufficient to see a meaningful effect.
Fluid management: Reducing caffeine and alcohol intake consistently improves storage symptoms — particularly urgency and nocturia. Both caffeine and alcohol are bladder irritants that increase detrusor overactivity. The timing of fluid intake also matters: reducing fluids in the two hours before bedtime specifically targets nocturia, which is often the most disruptive symptom.
Pelvic floor exercises: Kegel exercises — contracting and holding the pelvic floor muscles — can improve urinary urgency and reduce post-void dribble in men with mild-to-moderate LUTS. They take six to eight weeks to show effect. They are particularly useful as first-line management before medication is considered.
What has weak or insufficient evidence
Lycopene (from tomatoes): Early observational data suggested a protective role against prostate cancer. Subsequent prospective trials have not confirmed a clinically significant benefit from lycopene supplementation [11]. Eating tomatoes as part of a Mediterranean-style diet is sensible; taking lycopene capsules is not supported by current evidence.
Saw palmetto: Widely marketed for prostate health. The largest randomised trial — the CAMUS trial — found no significant difference in IPSS scores between saw palmetto and placebo over 72 weeks [12]. Its continued popularity is a triumph of marketing over evidence. More dangerously, saw palmetto may lower PSA values, potentially masking a genuinely rising PSA and delaying cancer detection.
Zinc, selenium, and vitamin E: The SELECT trial — the largest prostate cancer prevention trial ever conducted, involving 35,533 men — found that vitamin E supplementation actually increased prostate cancer risk by 17% in healthy men [13]. Selenium showed no benefit. Neither supplement should be taken for prostate cancer prevention.
➡️ Related: Top 3 Prostate Supplements — What the Evidence Actually Says

Treatment Options: From Watchful Waiting to Surgery
If you have been diagnosed with BPH or a grey-zone PSA, understanding the treatment landscape before your urology appointment allows you to be an active participant in the decision rather than a passive recipient of it. Here is the framework I use in clinic:
For BPH
Which Treatment Pathway Fits Your Lifestyle?
Are you trying to preserve sexual function? Do you have a massive prostate? Before reading the medical options below, use our interactive tool to find the clinical pathway that aligns with your personal goals.
Watchful waiting is appropriate for men with mild symptoms (IPSS 0–7) and no complications. Annual monitoring with IPSS, flow rate, and post-void residual volume measurement is sufficient. No medication is required unless symptoms progress.
Alpha-blockers (tamsulosin, alfuzosin, silodosin) are the first-line medication for moderate symptoms. They relax the smooth muscle in the prostate and bladder neck, reducing urethral resistance. They work within 48–72 hours. They do not shrink the prostate and do not alter disease progression. Side effects include dizziness, nasal congestion, and — in about 10% of men — retrograde ejaculation (semen going backwards into the bladder at orgasm). An important and often missed interaction: if you take tamsulosin and you need cataract surgery, tell your ophthalmologist before the procedure — the drug causes intraoperative floppy iris syndrome (IFIS) that must be anticipated.
5-alpha reductase inhibitors (finasteride, dutasteride) block the conversion of testosterone to DHT and actually shrink the prostate by 20–30% over 6–12 months [3]. They reduce the risk of acute urinary retention by 57% and the need for surgery by 55% over four years — outcomes alpha-blockers cannot match. The trade-off: sexual side effects including erectile dysfunction (5–8%), reduced libido, and decreased ejaculate volume. They also halve the PSA value, so any urologist interpreting your PSA must know you are taking these medications.
Combination therapy with an alpha-blocker plus a 5-ARI is reserved for men with large prostates (>40 grams) and moderate-to-severe symptoms. The CombAT trial demonstrated a 41% reduction in symptom progression over four years compared to tamsulosin alone [14].
Surgery becomes the answer when medications fail, symptoms deteriorate, or complications develop — acute retention, recurrent UTIs, bladder stones, or kidney damage from back-pressure. TURP (transurethral resection of the prostate) remains the gold standard for prostates 30–80 ml, with 85–90% symptom improvement. HoLEP (holmium laser enucleation) is increasingly preferred for larger glands and in men on anticoagulants. For men who prioritise ejaculatory preservation, UroLift and Rezūm are office-based minimally invasive alternatives with lower re-treatment durability.
For prostate cancer
Active surveillance is the standard of care for low-grade prostate cancer (Gleason 6 / Grade Group 1). It involves structured monitoring — serial PSA, MRI, and periodic re-biopsy — with the intention to intervene only if the cancer shows signs of upgrading. The ProtecT trial showed cancer-specific mortality was below 1% at 10-year follow-up regardless of whether men received immediate treatment or were monitored [15]. Approximately 50–60% of eligible men avoid treatment entirely over a decade.
Radical prostatectomy (surgical removal of the prostate) or radiotherapy are offered for intermediate- and high-grade disease. Both carry significant side effect profiles — erectile dysfunction in 30–70% after radical prostatectomy, urinary incontinence in 5–20%, and bowel effects with radiotherapy. These are treatments for cancers that genuinely need treatment — not for the low-grade disease that active surveillance handles safely.
💡 In My Practice
The most consistent pattern I see in men over 40 presenting to my clinic is a long delay — symptoms that have been present for two to three years, gradually worsening, attributed to “normal ageing” or embarrassment about discussing urinary function. By the time they arrive, some of them have significant post-void residuals, early bladder wall thickening on ultrasound, and occasional episodes of near-retention. All of it entirely treatable — but advanced enough that simpler early-stage options are no longer appropriate.
The second pattern I see constantly is the man who walks in terrified about his PSA — having Googled his result and convinced himself he has advanced cancer — only to discover that his PSA of 5.8 is being driven by a 90-gram benign prostate and a PSA density of 0.06. His relief when I explain the 75% statistic — that three in four men in the grey zone have no cancer at all — is visible within the first five minutes. That relief could have been his two weeks earlier if the referral letter had included even one reassuring sentence.
⚠️ When to See a Doctor — Urgently
- Complete inability to urinate (acute urinary retention) — go to the emergency department immediately. A catheter will be placed to drain the bladder, and urgent urology referral will follow. Do not wait to see if “it passes”
- Fever with urinary symptoms — this combination may indicate acute bacterial prostatitis or an infected obstructed kidney. Both require same-day hospital assessment, IV antibiotics, and possibly emergency urinary drainage
- Visible blood in the urine (haematuria) — even a single episode of frank haematuria in a man over 40 should trigger same-day or next-day urgent urology referral to exclude bladder cancer, prostate pathology, or renal tumour
- New bone pain in the lower back, hips, or pelvis alongside a raised PSA — this may indicate metastatic prostate cancer and requires urgent investigation, not a routine outpatient slot
- PSA that has doubled in under 12 months — rapid PSA doubling time in the context of a known elevated PSA is one of the most clinically significant findings in prostate cancer risk stratification and warrants urgent urological assessment
Frequently Asked Questions
Does an enlarged prostate mean I’m more likely to get prostate cancer?
No. This is one of the most persistent and damaging misconceptions in men’s health. Benign prostatic hyperplasia (BPH) and prostate cancer are distinct conditions originating in different anatomical zones of the prostate. Having a large benign prostate does not increase your risk of cancer. It does, however, elevate your PSA — which is why PSA interpretation in the context of known BPH requires clinical expertise, not just a raw number. Never skip your PSA monitoring because you have BPH; the two conditions can coexist and one does not protect you from the other.
How do I know if my urinary symptoms are BPH or something more serious?
The symptom pattern is a starting point, not a definitive answer. Gradual-onset, progressive voiding symptoms — weak stream, hesitancy, nocturia — in a man over 50 with no other features strongly suggest BPH. However, blood in the urine, pelvic pain, rapid symptom onset, or any systemic features (weight loss, fatigue, bone pain) should not be attributed to BPH without investigation. A urology assessment including IPSS score, digital rectal examination, PSA, urinalysis, and ultrasound of the bladder for post-void residual is the minimum workup required to give you a confident answer.
Can I take saw palmetto for my prostate?
I understand why men reach for it — it is widely marketed, it carries a safe reputation, and the idea of a natural remedy is appealing. But the clinical evidence is clear: saw palmetto does not improve urinary symptoms beyond placebo. The CAMUS trial — a high-quality randomised controlled trial specifically designed to test this question — found no benefit whatsoever over 72 weeks [12]. More importantly, saw palmetto may lower your PSA, which could mask a genuinely rising level and delay detection of developing cancer. If you are taking saw palmetto, tell your urologist before your next PSA test.
Will prostate surgery affect my sex life?
It depends entirely on which procedure and why. For BPH surgery (TURP or HoLEP), the most common sexual change is retrograde ejaculation — semen entering the bladder at orgasm rather than being expelled externally. This occurs in 65–75% of men after TURP and is permanent. Orgasm sensation is preserved in most men. Erectile function is preserved in approximately 90–95% of cases. For men who prioritise ejaculatory function, UroLift and Rezūm are alternatives worth discussing before committing to TURP. For prostate cancer surgery (radical prostatectomy), erectile dysfunction is a significant risk — 30–70% depending on surgical technique, age, and pre-operative erectile function — and should be discussed in depth with your surgeon before proceeding.
What should I do right now if I’m a man over 40 who has never had a prostate check?
Book a GP appointment and ask for a prostate health discussion. This should include: a PSA blood test (after avoiding ejaculation and vigorous exercise for 48 hours), a digital rectal examination if appropriate for your age and risk profile, a brief urinary symptom assessment using the IPSS, and a family history review. If you have a father or brother who had prostate cancer, or if you are of African or Caribbean descent, make this appointment now — you may need to start screening earlier than the average-risk guidance suggests. The consultation takes 15 minutes. The information it generates could be clinically significant for the next 30 years.
📚 References
- Berry SJ, et al. The development of human benign prostatic hyperplasia with age. J Urol. 1984;132(3):474–479.
- McNeal JE. The zonal anatomy of the prostate. Prostate. 1981;2(1):35–49.
- McConnell JD, et al. The long-term effect of doxazosin, finasteride, and combination therapy on the clinical progression of benign prostatic hyperplasia. N Engl J Med. 2003;349(25):2387–2398.
- Rawla P. Epidemiology of prostate cancer. World J Oncol. 2019;10(2):63–89.
- Catalona WJ, et al. Measurement of prostate-specific antigen in serum as a screening test for prostate cancer. N Engl J Med. 1991;324(17):1156–1161.
- EAU Guidelines on Prostate Cancer. European Association of Urology. 2024 Edition.
- Schröder FH, et al. Screening and prostate cancer mortality: results of the ERSPC at 13 years of follow-up. Lancet. 2014;384(9959):2027–2035.
- Nickel JC, et al. Prevalence and impact of urological conditions for men in a Canadian epidemiological study. BJU Int. 2001;88(9):879–885.
- Giovannucci E, et al. Height, predictors of C-peptide, and cancer risk in the Physicians’ Health Study. Cancer Epidemiol Biomarkers Prev. 1997;6(8):641–648.
- Parsons JK, et al. Obesity and benign prostatic hyperplasia: clinical connections, emerging etiological paradigms and future directions. J Urol. 2009;182(6 Suppl):S27–31.
- Etminan M, et al. The role of tomato products and lycopene in the prevention of prostate cancer: a meta-analysis of observational studies. Cancer Epidemiol Biomarkers Prev. 2004;13(3):340–345.
- Barry MJ, et al. Effect of increasing doses of saw palmetto extract on lower urinary tract symptoms: a randomized trial (CAMUS trial). JAMA. 2011;306(12):1344–1351.
- Klein EA, et al. Vitamin E and the risk of prostate cancer: the Selenium and Vitamin E Cancer Prevention Trial (SELECT). JAMA. 2011;306(14):1549–1556.
- Roehrborn CG, et al. The effects of combination therapy with dutasteride and tamsulosin on clinical outcomes in men with symptomatic BPH: 4-year results from the CombAT study. Eur Urol. 2010;57(1):123–131.
- Hamdy FC, et al. 10-year outcomes after monitoring, surgery, or radiotherapy for localised prostate cancer (ProtecT trial). N Engl J Med. 2016;375(15):1415–1424.

Dr. Muhammad Khalid
MBBS · FCPS (Urology) · MCPS (Gen. Surgery) · CHPE · CRSM · IMC #539472
Specialist urologist with 11+ years of clinical experience across tertiary teaching hospitals. Trained at Lady Reading Hospital and Khyber Teaching Hospital, Peshawar. Author of 5 peer-reviewed international publications in Cureus, WJSA, and AJBS. Procedural expertise: URS, PCNL, RIRS, TURP, TURBT, and major open urological surgery. Full profile →
This article is for educational purposes only and does not constitute medical advice. Always consult your physician or urologist for diagnosis and treatment decisions specific to your condition.
