If you’re a man over 50 who gets up twice a night to urinate, waits at the toilet for the stream to start, and finishes with a dribble that requires an extra minute of patience — you probably have an enlarged prostate. And if you’ve been on medication for months or years and things aren’t improving, or they’ve started getting worse again, you’re asking the right question: when is it time for surgery?
Benign prostatic hyperplasia (BPH) — overgrowth of the prostate gland that is not cancer — affects roughly 50% of men by age 60 and up to 90% by age 85 [1]. It can significantly degrade quality of life, disrupt sleep, and in severe cases, damage the bladder and kidneys. The progression from “mild annoyance” to “I need something done about this” is gradual, which is exactly why many men wait too long.
As a urologist who manages BPH daily — from first prescriptions to operating theatre — I’m going to walk you through the complete treatment pathway: what medications do, when they stop working, and what your surgical options actually look like in 2026.
📋 Key Takeaways
- BPH is NOT cancer — it’s benign overgrowth of prostate tissue that squeezes the urethra and obstructs urine flow
- Alpha-blockers (tamsulosin) work within days and are first-line, but they do not shrink the prostate — they only relax the surrounding muscle
- 5-alpha reductase inhibitors (finasteride/dutasteride) actually shrink the prostate by 20–30% but take 6–12 months and can cause sexual side effects [5]
- Surgery becomes the answer when medications fail, symptoms worsen, or complications develop (retention, recurrent UTIs, bladder stones, kidney damage)
- TURP remains the gold standard surgical treatment, but laser procedures (HoLEP, GreenLight) offer lower bleeding risk and shorter hospital stays
- Retrograde ejaculation (semen entering the bladder at orgasm) occurs in 65–75% after TURP — this must be discussed honestly before surgery
Understanding BPH: What’s Actually Happening Inside
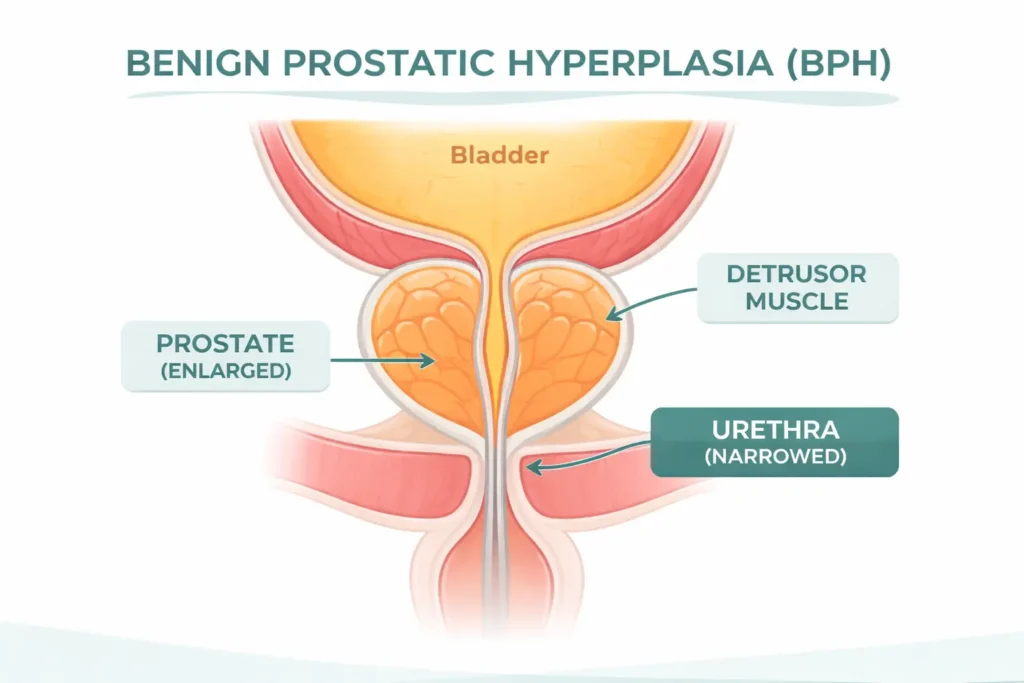
Your prostate sits just below your bladder, wrapped around the urethra like a ring around a pipe. Starting in your 40s, the central zone of the prostate begins to grow — slowly, silently, and in virtually all men. This growth is driven by dihydrotestosterone (DHT), a potent derivative of testosterone produced by the enzyme 5-alpha reductase within the prostate.
As the prostate enlarges, it compresses the urethra from the outside, creating resistance to urine flow. Your bladder compensates by working harder — the muscle wall thickens (detrusor hypertrophy), generating higher pressures to push urine through the narrowing channel. This compensation works for a while, which is why symptoms develop gradually rather than suddenly.
Eventually, the bladder muscle becomes overworked and begins to fail. That’s when incomplete emptying, overflow incontinence, and in the worst cases, bilateral hydronephrosis (backpressure damaging both kidneys) develop. This cascade — from minor nuisance to organ damage — can take years or decades, but it is progressive in a significant proportion of men [2].
The symptoms — what men actually experience
Urologists categorise BPH symptoms into two groups:
Storage symptoms (irritative — the ones that bother men most):
- Nocturia — waking 2+ times per night to urinate. Usually the symptom that finally drives men to seek help, because it destroys sleep quality
- Urgency — a sudden, compelling need to urinate that’s difficult to defer
- Frequency — urinating more than 8 times during the day
- Urge incontinence — leaking before reaching the toilet
Voiding symptoms (obstructive — the classic BPH signs):
- Weak stream — reduced force and calibre of the urinary stream
- Hesitancy — waiting or straining to start urination
- Intermittency — stream stops and starts during voiding
- Terminal dribbling — a slow trickle at the end
- Incomplete emptying — feeling like the bladder didn’t fully empty
- Straining — using abdominal pressure to push urine out
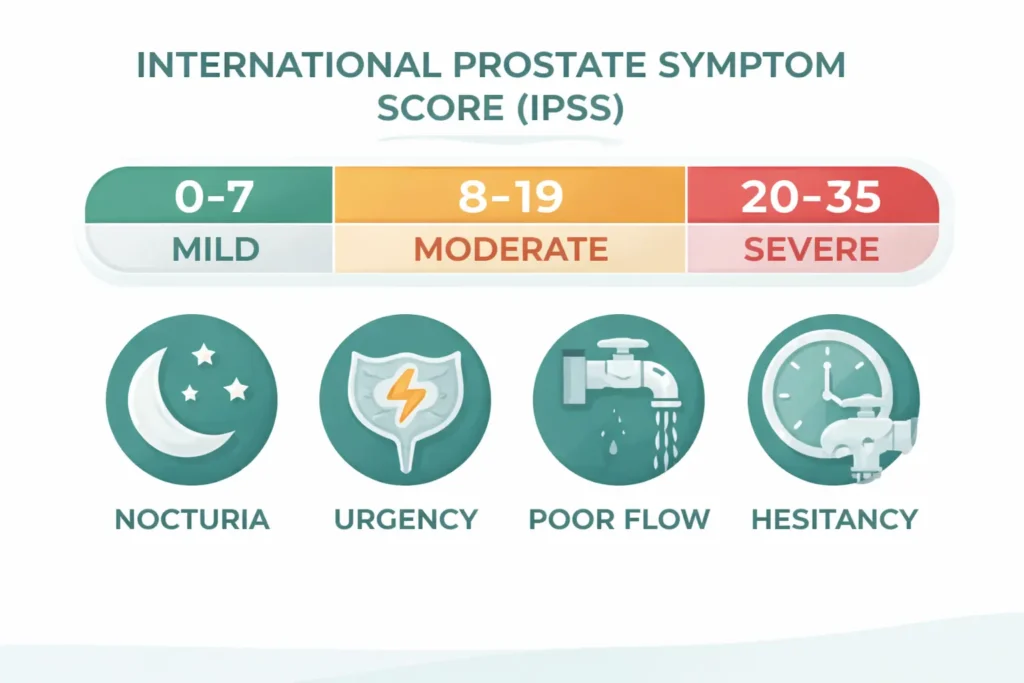
We quantify symptom severity using the International Prostate Symptom Score (IPSS) — a standardised 7-question tool scored 0–35. Mild: 0–7. Moderate: 8–19. Severe: 20–35. This score is tracked over time and is one of the key factors in deciding when to escalate treatment [3].
Stage 1: Medication — What It Does and What It Doesn’t
Most men with moderate BPH symptoms start with medication. There are two main drug classes, and understanding what each one actually does — and doesn’t do — is critical for setting realistic expectations.
Alpha-blockers: the quick relief option
Drugs: Tamsulosin (Flomax), alfuzosin, silodosin, doxazosin, terazosin
How they work: The prostate and bladder neck contain smooth muscle with alpha-1 adrenergic receptors. Alpha-blockers relax this muscle, reducing the dynamic (muscular) component of obstruction. They widen the channel without shrinking the prostate itself.
Onset: Symptom improvement within 48 hours to 2 weeks — the fastest-acting BPH treatment.
Effectiveness: Improve IPSS by 4–6 points on average. Increase peak flow rate by 2–3 ml/sec [4]. Very effective for mild-to-moderate symptoms.
Side effects to know about:
- Dizziness and orthostatic hypotension — especially with doxazosin and terazosin (non-selective). Tamsulosin is more prostate-selective and causes less blood pressure drop
- Retrograde ejaculation — semen goes backward into the bladder instead of forward. Occurs in about 10% with tamsulosin. Harmless but surprising if not warned
- Intraoperative floppy iris syndrome (IFIS) — if you need cataract surgery while on tamsulosin, tell your ophthalmologist. This is important and frequently missed
- Nasal congestion — minor but common
The limitation: Alpha-blockers do not stop prostate growth. They treat the symptom (obstruction) but not the disease (enlargement). Over time, as the prostate continues to grow, alpha-blockers become insufficient. They also don’t reduce the risk of acute urinary retention or the need for future surgery.
5-alpha reductase inhibitors (5-ARIs): the slow shrinkage option
Drugs: Finasteride (Proscar) and dutasteride (Avodart)
How they work: Block the conversion of testosterone to DHT — the hormone that drives prostate growth. Over 6–12 months, this actually shrinks the prostate by 20–30% [5].
Onset: Slow. Meaningful symptom improvement takes 3–6 months. Maximum effect at 12 months. This is the main reason patients abandon them — they expect the speed of tamsulosin and get frustrated.
Effectiveness: Reduce IPSS by 3–4 points. Reduce prostate volume by 20–30%. Crucially, reduce the risk of acute urinary retention by 57% and the need for surgery by 55% over 4 years — something alpha-blockers cannot do [5].
Side effects — the honest conversation:
- Erectile dysfunction — reported in 5–8% of men. Usually reversible on stopping the drug, though rare cases of persistent sexual dysfunction after discontinuation have been reported
- Decreased libido — 3–6%
- Reduced ejaculate volume — common
- Gynaecomastia (breast enlargement/tenderness) — rare but documented
- PSA reduction — finasteride/dutasteride halve your PSA value. Your doctor must know you’re taking these, otherwise a “normal” PSA could mask an elevated true value. Rule of thumb: multiply your PSA by 2 if you’re on a 5-ARI
Combination therapy: when one drug isn’t enough
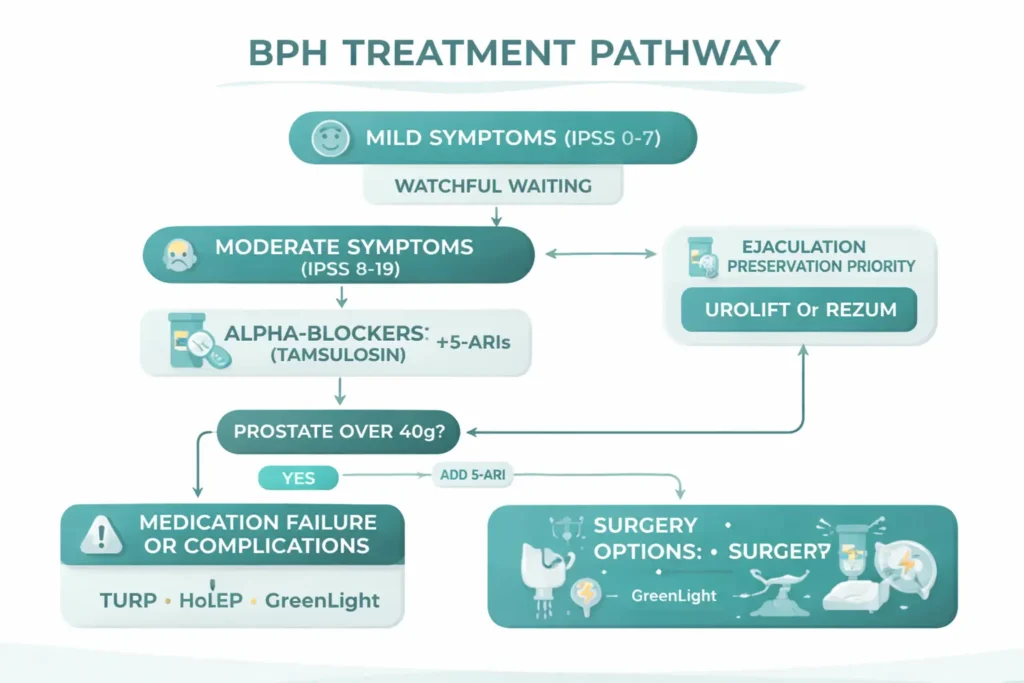
For men with moderate-to-severe symptoms AND a significantly enlarged prostate (>40 grams on ultrasound), combination therapy with an alpha-blocker + 5-ARI is more effective than either alone. The landmark CombAT trial demonstrated that combination therapy reduced the risk of symptom progression by 41% compared to tamsulosin alone over 4 years [6].
The trade-off is a higher side effect burden — you get the side effects of both drug classes. For this reason, combination therapy is reserved for men with genuinely large prostates who are at high risk of progression, not for mild symptoms.
➡️ Related Read: My PSA is 4.5 — Do I Have Cancer? Understanding Grey Zone Results
When Medication Fails: The 7 Signs It’s Time for Surgery
This is the question I get asked most often, and there’s no single universal answer — it depends on symptom severity, quality of life impact, and the presence of complications. Surgery should be seriously considered when:
- Acute urinary retention — you physically cannot urinate and require a catheter. If this happens more than once despite adequate medication, surgery is strongly indicated
- Recurrent urinary tract infections — caused by a chronically elevated post-void residual (urine left in the bladder after voiding). Stagnant urine breeds bacteria
- Bladder stones — form in stagnant residual urine. Their presence means the obstruction is significant enough to alter bladder chemistry
- Renal impairment — elevated creatinine with bilateral hydronephrosis on ultrasound means backpressure from the obstruction is damaging your kidneys. This is an urgent indication
- Recurrent gross haematuria — bleeding from engorged prostatic blood vessels that doesn’t settle with conservative measures
- Medication failure — symptoms persist or worsen despite optimised combination therapy for 6–12 months
- Quality of life — subjective but valid. If nocturia is destroying your sleep, if you can’t sit through a meeting without needing the toilet, if you’re planning your life around bathroom access — that’s reason enough if medication isn’t working
The Surgical Options: A Urologist’s Honest Comparison
TURP (Transurethral Resection of the Prostate) — the gold standard
TURP has been the reference standard for BPH surgery for over 80 years. A resectoscope is passed through the urethra (no external incisions), and the obstructing prostate tissue is shaved away using an electrically heated wire loop. The chips of tissue are irrigated out and sent for histological analysis.
- Best for: Prostate volume 30–80 ml (the majority of BPH cases)
- Success rate: 85–90% symptom improvement. Peak flow rate typically doubles or triples
- Hospital stay: 1–3 days with a catheter for 24–48 hours
- Recovery: Full recovery 4–6 weeks. Avoid heavy lifting and straining during this period
- Durability: Long-term results are excellent. Re-treatment rate approximately 1–2% per year [7]
Side effects of TURP:
- Retrograde ejaculation: 65–75% — the most common side effect. Semen enters the bladder during orgasm instead of being expelled externally. Orgasm sensation is preserved in most men, but there is no visible ejaculate. This is permanent and must be discussed before surgery
- Erectile dysfunction: 5–10% — often temporary, related to thermal or electrical injury near the neurovascular bundles
- Urinary incontinence: 1–3% — usually mild and temporary. Severe permanent incontinence is rare (<1%)
- Bleeding requiring transfusion: 2–5% — higher with larger prostates
- TUR syndrome: Rare with modern bipolar TURP (uses saline irrigation). Was more common with older monopolar technique
- Urethral stricture: 2–5% — narrowing of the urethra from instrumentation, may require dilation
HoLEP (Holmium Laser Enucleation of the Prostate) — the modern challenger
HoLEP uses a holmium laser to enucleate (shell out) entire lobes of the prostate from within, rather than shaving tissue piece by piece like TURP. The enucleated tissue is pushed into the bladder, morcellated (cut into fragments), and removed.
- Best for: Any prostate size — including very large prostates (>80–100 ml) where TURP becomes risky. HoLEP is size-independent, which is its biggest advantage
- Success rate: Equivalent to or better than TURP for symptom relief
- Hospital stay: Often shorter than TURP — many centres discharge within 24 hours
- Bleeding risk: Significantly lower than TURP — the laser cauterises as it cuts. Suitable for men on anticoagulants
- Durability: Excellent — re-treatment rate is very low because the adenoma is completely removed, not just debulked
The catch: HoLEP has a steep surgical learning curve — a urologist needs approximately 50 cases to become proficient [8]. Not all centres offer it, and outcomes are highly surgeon-dependent. If your urologist performs HoLEP regularly, it’s an excellent option. If they’ve done fewer than 20 cases, consider travelling to a high-volume centre.
GreenLight (PVP — Photoselective Vaporisation of the Prostate)
Uses a high-powered KTP or LBO laser to vaporise prostate tissue on contact, creating an immediate channel.
- Best for: Small to medium prostates (30–80 ml). Men on anticoagulants (lowest bleeding risk of all surgical options)
- Advantages: Very low bleeding risk, often same-day discharge, shorter catheter time
- Disadvantages: No tissue specimen for histology (tissue is vaporised, not removed). Slightly higher re-treatment rate compared to TURP and HoLEP. Can cause irritative voiding symptoms for several weeks post-operatively
Newer minimally invasive therapies (MISTs) — for ejaculatory preservation
Several newer procedures aim to preserve ejaculatory function — a major concern for sexually active men:
- UroLift (prostatic urethral lift): Small implants hold the enlarged lobes apart, like curtain tie-backs. Preserves ejaculation in most men. Best for small-to-moderate prostates without a median lobe. Re-treatment rates of 13.6% at 5 years [9]
- Rezūm (water vapour therapy): Steam is injected into the prostate, causing targeted cell death and shrinkage over weeks. Preserves ejaculation in most. Takes 2–4 weeks for symptom improvement
- Aquablation: Robot-guided waterjet ablation using ultrasound mapping. Shows promise for larger prostates with lower retrograde ejaculation rates than TURP. Still relatively new with limited long-term data
Open prostatectomy (simple prostatectomy)
Reserved for very large prostates (>80–100 ml) in centres where HoLEP is not available. An abdominal incision is made and the adenoma is shelled out by hand. Highly effective but carries higher morbidity — longer hospital stay (3–5 days), more bleeding, longer recovery. Increasingly being replaced by HoLEP and robotic-assisted simple prostatectomy.
➡️ Related Read: Prostate Cancer Screening — The Age-by-Age Guide Every Man Needs
What to Expect After Prostate Surgery
Recovery after TURP or laser prostate surgery follows a predictable pattern, but patients are often surprised by some aspects:
- Week 1–2: Catheter removed (usually 24–48 hours post-op). Urination may burn initially. Urine may be blood-tinged — this is normal and can last 2–4 weeks. Drink plenty of fluids to keep urine dilute
- Week 2–4: Frequency and urgency often temporarily worsen before they improve. This is counterintuitive and alarms many patients, but it happens because the raw prostatic bed is healing and the bladder is readjusting to lower resistance
- Week 4–6: Stream should be noticeably stronger. Nocturia improving. Most men can return to normal activity. Avoid heavy lifting (>10 kg) until cleared by your surgeon
- Month 3: Full benefit is usually apparent by this point. IPSS should be significantly lower than pre-surgery
- Long-term: Annual follow-up with flow rate and residual volume measurement. PSA monitoring continues — BPH surgery does NOT eliminate the need for prostate cancer screening

💡 In My Practice
The most common pattern I see is a man in his early 60s who’s been on tamsulosin for 2–3 years. It worked well initially, but over the past year his nocturia has crept back to 3–4 times per night, his stream has weakened again, and he’s starting to have significant post-void residuals on ultrasound. His prostate has continued growing despite the alpha-blocker. This is the classic point where we have the surgery conversation.
The biggest barrier to timely surgery in my practice is fear — specifically, fear of incontinence and impotence. When I explain that the actual risk of permanent incontinence after TURP is under 1%, and that ED risk is 5–10% (and often temporary), most men are surprised. They’d imagined much worse. The conversation about retrograde ejaculation requires more careful handling — for sexually active men, the idea of a “dry orgasm” is distressing, and I always discuss ejaculation-preserving alternatives (UroLift, Rezūm) for men where this is a priority.
What I wish more patients knew: if you wait until you’re in acute retention with a catheter, you’ve already developed bladder damage that may not fully recover even after successful surgery. The men who do best are those who have surgery while their bladder still has good contractile function — not after years of overdistension have compromised it.
⚠️ When to See a Doctor — Urgently
- Complete inability to urinate (acute urinary retention) — go to the emergency department. A catheter will be placed to drain the bladder, and you’ll be referred to urology for definitive management
- Visible blood in urine (haematuria) — especially if accompanied by clots. May indicate prostatic bleeding or the need to exclude bladder cancer
- Fever with urinary symptoms — may indicate UTI secondary to incomplete emptying, or acute prostatitis
- Pain in the lower back or flanks with reduced urine output — may suggest bilateral obstruction affecting the kidneys (hydronephrosis)
See your GP or urologist (non-urgent appointment) if:
- You’re getting up 2+ times per night to urinate regularly
- Your stream has become noticeably weaker over months
- You feel your bladder doesn’t empty completely
- BPH medications that once worked are becoming less effective
- You’re taking tamsulosin and you need cataract surgery (intraoperative floppy iris syndrome risk — tell your ophthalmologist)
Download Your Free Clinical Action Plan
Enter your email below to download Dr. Khalid’s complete BPH & Prostate Screening Guide as a free, printable PDF.
Frequently Asked Questions
Does BPH increase my risk of prostate cancer?
No. BPH and prostate cancer are separate conditions. Having an enlarged prostate does not increase your cancer risk. However, both conditions become more common with age and can coexist. BPH can elevate PSA levels, which complicates cancer screening — this is why PSA interpretation requires urological expertise, not just a number on a lab report.
Can I take tamsulosin forever?
You can take it long-term, and many men do for years. However, it doesn’t prevent disease progression. If your symptoms are well-controlled, your residual volumes are low, and your kidneys are normal, long-term tamsulosin is a reasonable strategy with regular monitoring — annual IPSS, flow rate, and residual volume measurement should all be tracked.
Will BPH surgery affect my sex life?
Retrograde ejaculation is the most common sexual change after TURP and HoLEP (65–75%). Orgasm sensation is usually preserved but there is no visible ejaculate. Erectile function is preserved in 90–95% of men. For men who prioritise ejaculatory preservation, UroLift and Rezūm are alternatives worth discussing — though their symptom relief is generally less dramatic than TURP for moderate-to-severe disease.
How do I choose between TURP, HoLEP, and laser surgery for BPH?
In practice, the choice often depends on what your urologist is most experienced with and what equipment is available at your hospital. For prostates under 80 ml, TURP, HoLEP, and GreenLight all produce excellent results. For very large prostates (>80–100 ml), HoLEP or open prostatectomy are preferred. Ask your surgeon how many of each procedure they’ve performed — surgical volume correlates strongly with outcomes.
Can BPH come back after surgery?
Regrowth is possible but uncommon. After TURP, the re-treatment rate is approximately 1–2% per year [7]. After HoLEP, it’s even lower because the entire adenoma is removed. If symptoms recur years after surgery, the cause may be bladder dysfunction (detrusor failure) rather than prostatic regrowth — urodynamic assessment is needed to differentiate.
📚 References
- Berry SJ, et al. The development of human benign prostatic hyperplasia with age. J Urol. 1984;132(3):474–479.
- Speakman MJ, et al. Lower urinary tract symptoms suggestive of benign prostatic hyperplasia (LUTS/BPH): more than treating symptoms? Eur Urol Suppl. 2008;7(11):680–689.
- Barry MJ, et al. The American Urological Association symptom index for benign prostatic hyperplasia. J Urol. 1992;148(5):1549–1557.
- Djavan B, Marberger M. A meta-analysis on the efficacy and tolerability of alpha-1 adrenoceptor antagonists in patients with LUTS suggestive of BPH. Eur Urol. 1999;36(1):1–13.
- McConnell JD, et al. The long-term effect of doxazosin, finasteride, and combination therapy on the clinical progression of benign prostatic hyperplasia. N Engl J Med. 2003;349(25):2387–2398.
- Roehrborn CG, et al. The effects of combination therapy with dutasteride and tamsulosin on clinical outcomes in men with symptomatic benign prostatic hyperplasia: 4-year results from the CombAT study. Eur Urol. 2010;57(1):123–131.
- EAU Guidelines on Management of Non-neurogenic Male LUTS. European Association of Urology. 2024.
- Elzayat EA, Elhilali MM. Holmium laser enucleation of the prostate (HoLEP): the endourologic alternative to open prostatectomy. Eur Urol. 2006;49(1):87–91.
- Roehrborn CG, et al. Five year results of the prospective randomized controlled prostatic urethral L.I.F.T. study. Can J Urol. 2017;24(3):8802–8813.

Dr. Muhammad Khalid
MBBS · FCPS (Urology) · MCPS (Gen. Surgery) · CHPE · CRSM · IMC #539472
Specialist urologist with 11+ years of clinical experience across tertiary teaching hospitals. Trained at Lady Reading Hospital and Khyber Teaching Hospital, Peshawar. Author of 5 peer-reviewed international publications in Cureus, WJSA, and AJBS. Procedural expertise: URS, PCNL, RIRS, TURP, TURBT, and major open urological surgery. Full profile →
This article is for educational purposes only and does not constitute medical advice. Always consult your physician or urologist for diagnosis and treatment decisions specific to your condition.
